An anal fissure is a small ulcer just inside the anal canal. They usually occur in just one place, but heal and return over many months or years. The continuing irritation nearby causes the skin next to it to become lumpy, leaving a skin tag. That piece of skin is mistaken by many people for a haemorrhoid. Anal fissure can occur at any age, but I have often seen it in young adults. A fissure may appear for no apparent cause, or it can be caused by an abrupt change in bowel habits, like constipation (in this case, meaning hard stool) or diarrhoea.
It seems that the ulcer (fissure) is caused by the tight contraction of the cylindrical muscles around the anal canal – much tighter and longer than normal. This muscle cramp might stop fresh blood from bringing oxygen to the lining of the anus, resulting in the breakdown (or ulceration) of that lining. The pain is probably from the muscle cramp, rather than from the ulcer.
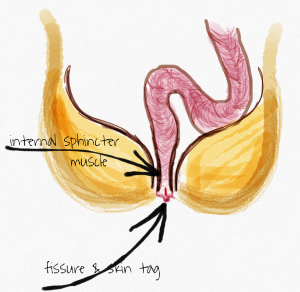
This picture of a slice through the anal canal shows the inner muscle layer (and an outer muscle layer, which is not affected) in brown. The little red fissure on the back wall of the anal canal might be caused by the inner muscle squeezing it too tight.
How do I know i have one? Typically, a fissure causes pain, most severe when triggered by passing a bowel motion, and sometimes bright bleeding can be seen on the toilet paper.
Most of the time, the fissure will heal by itself, and this can be helped by ensuring that the stools are formed, but soft. Prevent constipation by drinking plenty of water, and eating fruit and plenty of fibre. Regular exercise is also very helpful – walking seems to stimulate the bowels to work more effectively. Some people also find things at the pharmacist to soften the stool, but try to avoid the tablets that stimulate the bowel contractions. We don’t want to push the hard stools faster – we want them to be soft and easy.
The usual “haemorrhoid creams” contain local anaesthetic, and so they might help a little, but they won’t make it heal any faster. There are specific creams which might actually allow the fissure to heal more quickly. In Perth, Rectogesic can be bought over the counter in your local pharmacy. It contains GTN, which causes the smooth muscle to relax. The same type of muscle is also present in your blood vessels, so if you absorb much of it into your system, you can suffer a low blood pressure when you stand up, or develop headaches. It is a good idea to use a very small amount at first, to allow your body to adapt to the new medication gradually. You will want to cover the skin around the anus over a radius of about a centimetre, but you also need to get the cream to the inner surface of the muscle, by putting you (gloved!) finger inside and twisting – so that you get at least the tip right inside.
Other creams can be made by Compounding Pharmacies – these might include Diltiazem or Nifedipine. However, you will need a prescription for these. Studies suggest that they are just as effective as Rectogesic, but may cause fewer headaches.
If keeping the stools soft, using the muscle-relaxing creams is not effective after six weeks, it might be worth considering paralysis of the muscle. This is done with an injection of Botulinum toxin, a procedure usually done under a general anaesthetic. It often results in a temporary risk of incontinence, but there are reports of permanent reduction in the effectiveness of control of the anus.
The traditional surgical treatment for anal fissure is cutting the lowest one third of the muscle. This is permanent, and if too much muscle is cut, there can be permanent loss of control of gas, or liquid stool, or sometimes even solid stool. Therefore, if surgical intervention is required for anal fissure, it is strongly recommended that a specialist colorectal surgeon is consulted.
Sue Taylor is not a colorectal surgeon.







One response to “What is an Anal Fissure?”
[…] Hernia Reflux Anal fissure […]